Introduction
Sodium hyaluronate, the salt form of hyaluronic acid, is a naturally occurring polysaccharide group of sugar in the human body. It is a popular ingredient in skincare and cosmetics due to its ability to hydrate and plump the skin. This sodium salt also has a wide range of applications in the medical field, particularly in anterior segment eye surgery. In this article, we will discuss the utilization and benefits of sodium hyaluronate in anterior segment surgery.
What Is Anterior Segment Surgery?
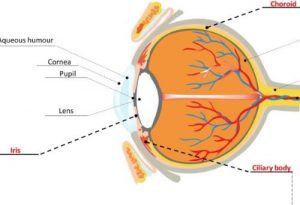
Anterior segment surgery involves operating on the structures in the front of the eye, such as the cornea, iris, and lens. These surgeries can range from cataract removal to corneal transplants. It is crucial to maintain the clarity of the cornea and the surrounding tissues to ensure a successful outcome. Sodium hyaluronate can play an essential role in achieving this. [caption id="attachment_9073" align="alignnone" width="300"] Human Eyes[/caption]
Human Eyes[/caption]
Benefits of Sodium Hyaluronate Employed in Anterior Segment Surgery
Sodium hyaluronate is a natural substance largely found in the extracellular matrix of connective tissues. It is in the aqueous humor and the vitreous, and it forms a protective coating on the corneal endothelium. Sodium hyaluronate and other viscoelastic substances, such as chondroitin sulfate and collagen, have been used for eye surgeries since the 1970s. These viscoelastic agents are used to protect and maintain the shape of the eye during surgery. They help create space for the surgeon to work and prevent damage to delicate structures as well.
--Maintaining A Deep Anterior Chamber
The primary benefit of using this salt as a viscoelastic agent is its ability to maintain a stable anterior chamber during the operation. The anterior chamber is the fluid-filled space between the cornea and the iris, and maintaining its stability is essential for successful surgery. Sodium hyaluronate can help stabilize the anterior chamber by providing a cushioning effect and preventing the collapse of the chamber. Therefore, it is easier to separate and maneuver these tissues, and the damage to the cornea and other tissues can be minimized.
--Protecting the Corneal Endothelium
Besides, the excellent lubricating properties of sodium hyaluronate can help reduce the risk of damage to the corneal endothelium during surgery. The corneal endothelium is a layer of cells that lines the back of the cornea, which is crucial for maintaining corneal clarity. Damage to the corneal endothelium can result in complications such as corneal edema and decreased vision. If it got scratched, there would be serious vision problems because all light passes through it and any defect might lead to a “blind spot”.
--No Adverse Effect
Sodium hyaluronate is a substance widely present in the human body, and there is no report on its adverse effects. So, it is considered to have no adverse effects and is safe to take. It is also biocompatible, meaning it is well-tolerated by the body and does not cause adverse reactions. Moreover, sodium hyaluronate can be easily absorbed by the body and does not require removal after surgery. Sodium hyaluronate is available in various forms, including gels, solutions, and ointments. The choice of form depends on the specific needs of the surgery and the surgeon's preference.
There is a variety of medical-grade sodium hyaluronates on our website. Send us an inquiry if you are interested. Related reading: Medical-grade Sodium Hyaluronate Guide 2023: Functions & Applications
Examples of Sodium Hyaluronate Used in Anterior Segment Surgery
You can find sodium hyaluronate as a surgical aid during ophthalmic surgeries including cataract extraction, corneal transplant, glaucoma infiltration, and intraocular lens implantation. With sodium hyaluronate products, the safety and reliability of anterior segment eye surgeries have been improved.
--Cataract Operations
Sodium hyaluronate was used as a surgical device for two cataract surgeries: intracapsular cataract extraction (ICCE) with corneoscleral incision and corneal incision. There were 80 patients divided in two groups. The first group used sodium hyaluronate products, while the control group employed a balanced salt solution (BSS) instead. It was proven that this sodium salt has a protective effect on the cornea and no side effects, such as intraocular pressure or inflammatory reaction, have been observed. [2]
--Intraocular Foreign Body (IOFB)
Diverse surgical instruments have been employed to remove intraocular foreign bodies (IOFBs). A 38-year-old healthy man suffered from a glass IOFB in the left eye after a glass exploration. Medical-grade sodium hyaluronate gel was used to remove the IOFB, which could avoid damage to the retina and make it easier to grasp the flat glass fragment. [3]
Conclusion
In a word, sodium hyaluronate is a useful tool in anterior segment surgery. Its viscoelastic properties can help maintain a stable anterior chamber and protect delicate structures during surgery. Its lubricating properties can reduce the risk of damage to the corneal endothelium, and its biocompatibility makes it a safe choice for use in surgery. If you are undergoing anterior segment eye surgery, be sure to discuss the use of sodium hyaluronate with your surgeon and learn about how it can benefit your surgery.
Stanford Chemical Company is a leading supplier of medical-grade sodium hyaluronate. Cosmetic grade, food grade, and injection grade are also available. Check our homepage to look for the perfect sodium hyaluronate products for your projects.